The physicians at Siva Orthopaedic Clinic provide world-class clinical excellence on an individual level with a human touch. They specialise in a range of procedures such as computer-assisted and minimal invasive surgery, arthroscopic “key hole” surgery and joint sparing procedures. Click on the below tabs to know more about their services.
-
- Total Knee Replacement
- Unicondylar Knee Replacement
- Patellofemoral Knee Replacement
- Computer Guided Knee Replacement
- Revision Knee Replacement
-
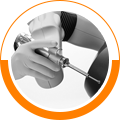
Robotic-assisted knee replacement surgery is an alternative to the conventional knee replacement procedure. It is performed using robotic-arm technology that allows your surgeon to precisely perform the surgery through a smaller incision as compared to traditional surgery.
-
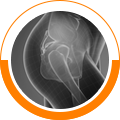
A bone fracture is a medical condition in which a bone is cracked or broken. It is a break in the continuity of the bone. While many fractures are the result of high force impact or stress, bone fracture can also occur as a result of certain medical conditions that weaken the bones, such as osteoporosis.
-
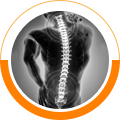
Sports injuries occur when playing indoor or outdoor sports or while exercising. Sports injuries can result from accidents, inadequate training, improper use of protective devices, or insufficient stretching or warm-up exercises. The most common sports injuries are sprains and strains, fractures, and dislocations.
If you wish to be advised on the most appropriate treatment, please call to schedule an appointment or click to request an appointment online.